Bariatric Equipment: How To Remarkably Support Safe Patient Movement

Providing quality care for bariatric (obese) patients poses unique challenges for healthcare workers. Safe patient handling and mobility are especially difficult when caring for larger patients.
Fortunately, specialised bariatric equipment can make a big difference in maintaining the safety and dignity of both patients and staff.
This article explores the lists of bariatric equipment available and best practices for its use in healthcare settings.
Table of contents
- What is Bariatric Equipment?
- The Risks of Mobilising Bariatric Patients Manually
- Benefits of Bariatric Equipment
- Common Bariatric Equipment and Uses
- How to Select Suitable Bariatric Equipment
- Special Considerations for Proper Bariatric Slings and Lifts
- Advice for Safely Using Bariatric Transfer Aids
- Implementing a Bariatric Handling Program
- Infection Control Considerations for Bariatric Equipment
- Training Considerations for Proper Bariatric Equipment Utilisation
- Creating a Dedicated Bariatric Handling Team
- Special Populations and Conditions Requiring Customised Bariatric Mobility Solutions
- Adapting Bariatric Equipment Strategies for the Home Setting
- Improving Bariatric Mobility Equipment Through Iteration and Data
- Perspective from Nurses on Bariatric Safe Patient Handling
- Key Takeaways on Bariatric Mobility Solutions
What is Bariatric Equipment?
Bariatric equipment refers to mobility aids and assistive devices specifically designed to accommodate larger, heavier individuals.
Standard hospital beds, wheelchairs, stretchers, and other equipment are typically not suitable for patients over 350 lbs.
Using undersized equipment can cause discomfort, skin breakdown, falls, and injuries. It also often takes more staff and effort to move obese patients without proper equipment.
Bariatric equipment is engineered with wider dimensions, higher weight capacities, and more durable frames. It aims to provide safe support, efficient movement and handling, skin integrity, and dignified care.
Common types of bariatric equipment include:
- Beds: pressure-reducing surfaces, powered functionality.
- Wheelchairs: wider frames, bariatric-strength materials.
- Stretchers and trolleys: increased clearance, 500-1000 lb capacity.
- Walkers, canes, crutches: reinforced designs.
- Lifts and slings: powered standing or full-body slings.
- Commodes, shower chairs: wider, sturdier seats.
- Floor lifts: powered lifting harness for floor transfers.

The Risks of Mobilising Bariatric Patients Manually
Attempting to move, lift, or reposition larger patients manually leads to preventable harm:
For patients:
- Fall risks due to unsteady manoeuvring or inadequate staff.
- Skin shearing, friction injuries, and bruising.
- Discomfort, loss of dignity, and psychological distress.
- Tubing and line dislodgement if grasped tightly.
- Joint dislocations from improper lifting techniques.
For caregivers:
- Career-ending back injuries from repeated heavy lifts and shifts.
- Neck, shoulder, and wrist strains from bearing weight incorrectly.
- Knee and hip damage from using poor body mechanics.
- Fatigue leading to judgement lapses and accidents.
- Moral distress when unable to move patients properly.
Specialised bariatric equipment eliminates unnecessary strain and struggle during handling. Improper ad hoc techniques place patients and staff at risk.
Benefits of Bariatric Equipment
- Safer for patients: Obesity puts patients at higher risk for falls and injuries during transfers and repositioning. Bariatric equipment is designed to protect patients up to 1000 lbs. Appropriate equipment also helps prevent discomfort and skin breakdown.
- Safer for staff: Manually lifting or moving a heavier person exponentially increases the risk of back, muscle, and joint injuries for staff. Bariatric equipment reduces strain and the need for multiple staff to assist.
- Supports dignity and independence: Patients may feel vulnerable or embarrassed when needing extra staff to help move them. Bariatric equipment allows self-transfers or minimises handling by others.
- Improves quality of care: Easier mobility supports better hygiene, prevents complications of immobility, and allows staff to focus on medical care versus physical maneuvers.
- Potential cost savings: Although bariatric equipment has higher upfront costs, it can reduce worker injuries, staffing needs, and lawsuits over time. This equipment also helps prevent costly medical complications.
Common Bariatric Equipment and Uses
Now let’s explore some of the most helpful bariatric equipment for safe patient handling:
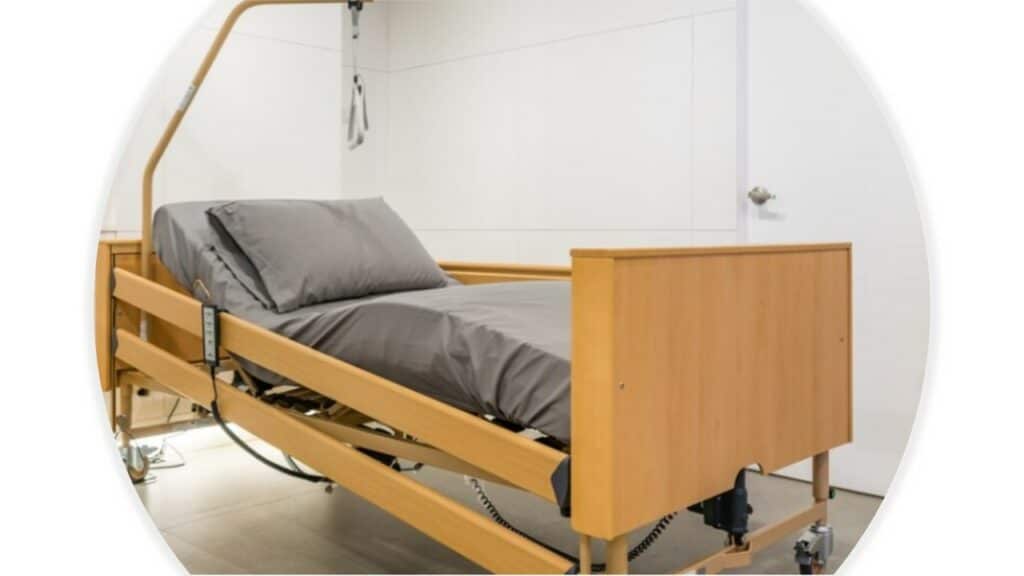
1. Beds
Bariatric beds offer expanded surface area and weight capacity for patient comfort.
Electric versions allow height and position adjustments with the touch of a button.
This assists staff with tasks like wound care without strenuous lifting.
Features like expandable wings and lateral rotation can ease body positioning for cleaning or surgery prep.
Low air loss and alternating pressure relieve pressure points and improve circulation.
2. Wheelchairs
Extra width and reinforced frames accommodate larger patients up to 700 lbs. Features like reclining backrests, padded arms, and adjustable leg rests increase comfort during transport.
Power options reduce propulsion effort for staff. Removable desks, IV poles, and oxygen holders make wheelchairs suitable for longer-term use.
3. Stretchers
Bariatric stretchers and carts ensure safe transport within a facility. They have reinforced, 400-600 lb capacity frames. Extra clearance between sides allows easy access for caregivers.
Hydraulic lift columns facilitate adjusting height for transfers. Central locking with steer-and-roll manoeuvrability improves control.
Many feature tip-up backrests and retractable head/foot sections to aid patient positioning.
4. Sit-to-Stand Lifts
Sit-to-stand lifts with powered lifting up to 600 lbs help patients go from sitting to standing. This assists with transfers to chairs, wheelchairs, or commodes.
Oversize bases provide stability, while lifting straps support the torso. Foot plates and arm supports on some models boost safety.
For patients with more mobility, stand assist lifts offer support handles and lifts up to 300 lbs for stability when moving from bed to a standing position.
5. Ceiling Lifts
Ceiling lift systems involve motorised lift units mounted and operated from ceiling tracks. These allow a single caregiver to safely transfer a patient in and out of bed.
Straps attach to the patient from overhead, removing any manual lifting or leverage effort for staff.
Ceiling lifts can extend over a bedroom or cover an entire facility. They work best with compatible slings that cradle the patient’s body securely.
6. Floor Lifts
For floor-to-chair transfers, motorised mobile floor lifts provide a harness to cradle and raise patients up to 1000 lbs.
Caregivers control the lift motion and height using a handheld pendant. Some floor lift models fold compactly for easy storage when not in use.
Inflatable transfer aids like airsleds also help slide patients along floors without friction.
7. Walkers and Canes
Bariatric walkers have wider bases and reinforced frames to provide stability for those up to 700 lbs.
Extra height adjustments accommodate taller individuals. Some feature built-in seats for resting.
Bariatric canes offer sturdy support up to 500 lbs, with options like offset or platform bases for more stability.
8. Commodes and Shower Chairs
Expanded commodes and shower chairs allow easier, safer transfers on and off.
Oversized toilet seats and frames hold more weight, while added bars and handles boost patient manoeuvrability and sense of security.
Shower chairs with cut-out seats improve hygiene access. The addition of wheels or slider boards helps caregivers position these chairs.
9. Slings and Slide Boards
Transfer slings support and cradle the body to allow smooth moves in seated positions.
They attach securely to lift equipment but don’t restrict range of motion. Bariatric slings come in sizes up to 90 inches wide and 2,000 lb weight capacity.
Slide boards and transfer mats, placed under patients, also utilise momentum and low friction to help slide or reposition higher-weight patients in beds and chairs.
Related Post: Sliding Sheets For Patients: How to Use, Don’ts and UK Regulations.
Learn Practical People Moving & Handling – Book Now
How to Select Suitable Bariatric Equipment
Choosing appropriate bariatric-rated products prevents device failures and mishaps:
- Consult manufacturer sizing guidelines and weight limits for each product. Do not exceed.
- Measure weight and dimensions of patients using scales and tapes to identify appropriate device sizes.
- Take into account weight distribution and centre of gravity when sizing and positioning.
- Involve therapists early to determine proper equipment needs based on mobility and functional goals.
- Trial equipment with patients and get feedback before acquiring if possible.
- Select electrically powered mobility aids whenever feasible to reduce staff strain.
- Have backup equipment available in case of unexpected admissions above current device limits.
- Budget for widened corridors, doorways, ramps when renovating facilities used by larger patients.
With accurate sizing and staff training, bariatric-specific equipment safely accommodates patients above typical weight ranges seen.
Special Considerations for Proper Bariatric Slings and Lifts
Matching sling characteristics to patient needs ensures safe, comfortable transfers:
Slings
- Increased dimensions (width, length) to fit larger bodies without dangerous gaps.
- High maximum weight ratings (up to 1500lbs+/113kg+).
- Available styles (hammock, standing, hygiene access, limb support).
- Consider padding, head support and quick-release buckles.
Lifts
- Higher weight capacities (1000lbs+/454kg+ motors).
- Expanded lift bases for stability with larger patients.
- Longer booms extending over beds with adequate clearance.
- Charging indicators and equipment inspections between transfers.
- Emergency stop buttons or backup controls if power fails.
Improperly sized slings and inadequate lift capacities lead to catastrophic failures and falls. Selecting products rated for bariatric use protects all involved.
Also Read: Moving and Handling Techniques- Essential Safer Handling of People
Advice for Safely Using Bariatric Transfer Aids
Regardless of the specific type, safe handling of bariatric transfer aids involves key considerations:
- Follow weight limits and size guidelines carefully to prevent equipment failures or tipping.
- Communicate thoroughly with patient before and during transfers.
- Use slow, gentle motions avoiding sudden shifts in weight distribution.
- Be prepared to quickly summon assistance if concerns of instability.
- Properly lock wheelchairs after transferring patient.
- Check skin after use for any damage or redness needing intervention.
- Ensure transfers aids remain clean – sanitise between patients.
- Provide transfers aids early in care to enable self-efficacy.
- Store equipment safely when not in use to prevent tripping risks.
With training, practice and team coordination, specialised aids enable smooth bariatric transfers without heavy lifting requiring multiple caregivers.
But staff should remain vigilant for any safety concerns requiring evaluation and optimisation.
Implementing a Bariatric Handling Program
To fully benefit from bariatric equipment, healthcare facilities should take a comprehensive approach:
- Form a bariatric handling committee to coordinate efforts.
- Research the right equipment choices for each unit and budget. Consider trial rentals or demos when possible.
- Develop clear protocols for equipment use, sling fit, cleaning, maintenance, and storage.
- Train all staff thoroughly on equipment use principles and policies. Stress the importance of using (versus avoiding) equipment.
- Identify appropriate equipment needs for each bariatric patient on admission. Proactively address positioning and mobility plans.
- Review policies and equipment choices regularly for potential upgrades.
- Address layout and accessibility challenges through expanding doorways, adding grip bars, managing cords, and ensuring sturdy furniture.
- Create a culture of safe handling where employees look out for each other’s injury prevention and feel comfortable voicing concerns.
With proper bariatric equipment and training, healthcare staff gain the tools and techniques to handle bariatric patients safely and respectfully.
The optimal result is better care experiences for this growing patient population.
In addition, with appropriate training, equipment and culture aligned, organisations can deliver consistently safe, dignified bariatric patient mobility.

Infection Control Considerations for Bariatric Equipment
Meticulous cleaning prevents contaminated bariatric equipment spreading pathogens:
General principles:
- Review manufacturer cleaning guidelines for proper techniques and approved disinfectants.
- Sanitise using facility-approved germicidal wipes or sprays between each patient.
- Wear proper PPE like gloves during cleaning and disassembly.
- Increase cleaning frequency for high touch surfaces like handgrips and control panels.
- Promptly remove any visible soil with absorbent materials then disinfect.
- Ensure thorough drying before returning to service.
Linens:
- Change lift slings even if barely used when moving between patients.
- Use disposable slings whenever feasible to simplify disinfection.
- Follow established laundering temperature and cycles for reusable slings.
Storage:
- Provide wall-mounted hooks near bariatric rooms for hanging lift slings between uses.
- Avoid sling storage on floors where they can become soiled.
- Use protective bags for clean linens to prevent inadvertent contamination.
Diligent cleaning after each use protects vulnerable bariatric patients and reduces risks of healthcare-associated infections.
Training Considerations for Proper Bariatric Equipment Utilisation
Thorough education protects patients and staff when using specialised mobility devices. Key points:
- Require completion of initial and annual refresher training for equipment.
- Hands-on practice sessions under supervision until proficiency confirmed.
- Tailor training to specific devices purchased by the organisation.
- Include weight limits, inspection procedures, cleaning/storage protocols.
- Review safe body mechanics for staff when operating lifts and transfers.
- Demonstrate use of attachments like wide straps and handling accessories.
- Highlight differences compared to standard equipment.
- Emphasise slow, gentle motion and smooth coordination between handlers.
- Welcome staff feedback on equipment to identify usability improvements.
With regular skills practice and peer education, safe bariatric equipment use becomes second nature. This reduces injury risks.
Creating a Dedicated Bariatric Handling Team
Given the specialised skills required, facilities utilising bariatric equipment often benefit from designated bariatric teams for moving and handling. Considerations when building these teams include:
- Assigning at least 4-6 core team members across shifts to ensure availability.
- Selecting staff with empathy, emotional intelligence and patience.
- Providing extensive initial equipment training and mentoring opportunities.
- Arranging for float pool staff to maintain competency by cross-training with the team periodically.
- Having the team serve as organisational equipment and policy resources.
- Recognising and celebrating team members to reinforce expertise and pride.
- Surveying all staff periodically on bariatric handling needs and concerns.
- Covering overhead lifting costs for bariatric team responses to urgent requests.
- Ensuring safe flooring, doorway, and bathroom dimensions for manoeuvres.
Developing excellent bariatric handling teams prevents injury while providing rewarding opportunities for staff interested in specialising.
Special Populations and Conditions Requiring Customised Bariatric Mobility Solutions
While standard bariatric equipment accommodates most patients, specialised needs warrant tailored solutions:
- Limited mobility patients may require total lift capability, including suspension vests.
- Wider pressure redistribution mattresses and limb protectors for advanced skin integrity risks.
- Custom lifts allowing precise positioning for procedures like dressing changes.
- Extra high weight capacity equipment for super bariatric patients.
- Enhanced infection control barriers for immunocompromised patients.
- Forearm instead of underarm crutch grips for some chronically obese users.
- Advanced facility renovations like floor cutouts and structural reinforcement to handle extreme bariatric cases.
Seeking input from therapists and the care team helps identify unique requirements needing customisation beyond routine bariatric equipment. But most needs are addressable.

Adapting Bariatric Equipment Strategies for the Home Setting
Safe at-home handling requires tailored solutions:
- Have therapists conduct home assessments checking doorway clearance, flooring, bathroom setup to identify mobility aid options and required modifications.
- Select lightweight, easily manoeuvrable home-use equipment if frequent relocation between rooms is needed.
- Arrange trial periods from medical equipment companies to test usability.
- Consider higher weight capacities even for standard mobility aids to provide use margin.
- Add grab bars, mobility rails, raised toilet seats and seating to boost independence.
- Provide caregiver education on special precautions like not stepping on wheel chocks when moving wheelchairs.
- Schedule additional home visits early on to adjust techniques and equipment as needed.
- Address accessibility barriers preventing home access to enable discharge.
With expertise and adapted supports, safe dignified handling is achievable even where hospital bed capacities and lifts are unrealistic.
Improving Bariatric Mobility Equipment Through Iteration and Data
Opportunities exist to continue advancing bariatric patient handling technology:
- Building patient mobility algorithms using smart lift data like forces and positioning to determine safest transfer motions.
- Force sensors ensuring lifts stay within safe working load limits during complex manoeuvres.
- Powered adjustable width transfer surfaces simplifying patient manoeuvring.
- Virtual reality simulation systems for bariatric training scenarios.
- Machine learning optimisation of lift strap position, anchor points, and motion for various tasks and body shapes.
- Mobile lift platforms allowing repositioning across settings without transfers.
- Improved beds and surfaces addressing the interplay between pressure injury risks and patient movement.
While already invaluable, equipment continues advancing through user feedback, data, and innovation to provide smoother, safer bariatric handling.

Perspective from Nurses on Bariatric Safe Patient Handling
Bariatric handling programs transform care experiences when implemented thoroughly.
Feedback from nurses at facilities utilising robust bariatric mobility protocols includes:
“Our organisation’s investment in suitable bariatric equipment like lifts, slings, beds, and flooring modifications has been life changing. We no longer fear crippling back injuries from improper manual lifts.”
“Having peer resources available who specialise in bariatric handling takes so much anxiety away. I know exactly who to call to handle larger patient mobilisation safely.”
“The bariatric slings allow me to provide hygiene and skin care for morbidly obese patients with minimal struggle or time. This preserves their dignity and my own health.”
“Our nursing retention has improved significantly since adopting formal safe bariatric handling practices. Nurses know their bodies will be protected.”
“With the improved bariatric floor lifts, I can safely rescue a fallen obese patient without having to bend and hurt my back. It gives great peace of mind.”
“I incorporated so many poor habits over the years without proper bariatric training and equipment before our new program. My body already feels less accumulated strain.”
“My frustrations with the lack of bariatric accommodations in the past still motivate me to generate ideas improving our resources and procedures. We can always do better.”
With training, support, and the right tools, safe dignified care becomes possible despite ongoing handling challenges.
But progress takes an organisational commitment to equipment, education, and culture building.
Key Takeaways on Bariatric Mobility Solutions
In summary, specialised mobility equipment eliminates unnecessary struggle and harm.
But comprehensive implementation through leadership priorities, budgets, training, and policies determines outcomes.
Success requires:
- Recognising bariatric manual handling risks.
- Budgeting for suitable weight-rated mobility aids.
- Appropriate sizing for comfort and function.
- Facility design accommodating manoeuvresExtensive training with ongoing refreshers.
- Developing expert peer handling resources.
- A culture focused on safe dignified movement
With forethought, teamwork, and the right tools, we can achieve safety for all while providing the high-quality care every patient deserves, regardless of body shape or size.
This vision calls healthcare workers to continue reaching higher together through constant improvement.
Let us Help you
We’ll help you find the right course for your needs. Tell us a little bit about your situation and what you would like to achieve.
We’ll get back to you within one working day.
