NMC Standards for Medicines Management: Ensuring Safe and Effective Patient Care
The management of medicines is a crucial aspect of healthcare delivery, as it directly impacts patient safety and the effectiveness of treatments. Nurses, as key members of the healthcare team, play a vital role in the administration, monitoring, and documentation of medication. To ensure high standards of care, the Nursing and Midwifery Council (NMC) has established comprehensive guidelines and standards for medicines management. In this blog post, we will explore the NMC standards for medicines management and their significance in ensuring safe and effective patient care.
Table of Content
- Understanding the Importance of Medicines Management
- Medicine Documentation and Communication
- Ensuring Compliance with NMC Standards
- Benefits of Adhering to NMC Standards for Medicines Management
- Medication Administration Record (MAR) Chart
- Medicine Management Challenges and Future Direction
- Conclusion on NMC Standards for Medicine Management
Understanding the Importance of Medicines Management
Medicines Management: An Essential Nursing Responsibility
Nurses play a vital role in medicines management. They are responsible for ensuring that patients receive the right medications, in the correct doses, and at the appropriate times. This includes:
- Collecting comprehensive medication histories
- Identifying patient-specific medication needs
- Planning and evaluating medication regimens
- Safely administering medications
- Monitoring and managing medication effects
- Documenting and communicating about medications
The Impact of Medication Errors on Patient Outcomes
Medication errors can have serious consequences for patient health and well-being. They can range from administering the wrong medication or dosage to failing to recognize drug interactions or allergies. Such errors can lead to adverse drug reactions, prolonged hospital stays, and even life-threatening situations. That’s why medicines management is of utmost importance.
By adhering to proper medicines management practices, nurses can significantly reduce the occurrence of medication errors. Thoroughly assessing patients’ medical histories, cross-checking prescriptions, and verifying medication orders are crucial steps that help ensure the right medication is given to the right patient. Additionally, monitoring patients for any adverse reactions or changes in their condition is essential for timely intervention and appropriate adjustments to the medication regimen.
The Role of Nurses in Medicines Management
Nurses play a vital role in medicines management throughout the healthcare journey. From the moment patients enter the healthcare facility, nurses are involved in collecting comprehensive medication histories, identifying patient-specific medication needs, and evaluating the effectiveness of the prescribed treatment plans.
When it comes to medication administration, nurses act as the link between healthcare professionals and patients. We are responsible for verifying medication orders, ensuring the correct administration technique, and applying the “Five Rights” of medication administration: right patient, right medication, right dose, right route, and right time. By following these principles, we minimize the risk of errors and maximize patient safety.
Moreover, nurses are continually monitoring and managing the effects of medications on patients. This involves assessing and documenting therapeutic responses, identifying and managing any adverse reactions, and promptly addressing medication errors or discrepancies. By being vigilant and proactive, nurses contribute to improved patient outcomes and help prevent potential complications.
In addition, medicines management is a critical responsibility for nurses. We understand the importance of ensuring the safe and effective use of medications, as errors in this area can have significant repercussions for patients.
By carefully managing medications, adhering to proper protocols, and being diligent in our documentation, we contribute to the overall well-being and safety of the individuals in our care.
Together, we can make a difference in enhancing patient outcomes through diligent and effective medicines management.

It is estimated that avoidable harm from medication errors costs the NHS £98 million annually and contributes to over 1,700 deaths.
Image by zinkevych on Freepik
Overview of NMC Standards for Medicines Management
The NMC (Nursing and Midwifery Council) has established standards for medicines management to ensure safe and effective practices in healthcare settings. These standards are based on the following principles:
- Competence: Nurses must demonstrate knowledge and understanding of medications, including their uses, side effects, and potential interactions.
- Accountability: Nurses are responsible for their own actions and decisions related to medicines management.
- Communication: Nurses must communicate effectively with patients, healthcare professionals, and other members of the healthcare team about medications.
- Documentation: Nurses must document all aspects of medicines management accurately and legibly.
- Safety: Nurses must take all necessary steps to ensure the safe and effective use of medications.
LIMITED TIME OFFERS – e-LEARNING CLINICAL COURSES- CPD APPROVED CERTIFICATE
How to Comply with NMC Standards for Medicines Management
There are a number of things nurses can do to comply with NMC standards for medicines management. These include:
- Attending regular training and continuing education courses to maintain their knowledge and skills related to medicines management.
- Participating in medication safety audits and reviews to identify and address areas of risk.
- Developing and implementing evidence-based policies and procedures for medicines management.
- Providing regular feedback to patients and their families about their medications.
- Reporting any medication errors or concerns to their manager or supervisor.
With these steps, nurses can help ensure that patients receive the safe and effective medications they need to improve their health and well-being.
FACE TO FACE – SAFER HANDLING OF MEDICATION TRAINING – SEE AVAILABLE DATES AND PRICE
Medicine Documentation and Communication
Accurate documentation and effective communication are essential for seamless medicines management. Let’s explore the key aspects of documentation and communication in medicines management.
Accurate Medication Documentation
Nurses are responsible for accurately documenting all aspects of medication administration, including the medication administered, the dosage, the route of administration, and the patient’s response. Clear and detailed documentation ensures continuity of care, promotes effective communication among the healthcare team, and serves as a legal record of the patient’s treatment.
Here are some tips for accurate medication documentation:
- Use the patient’s full name and date of birth.
- List the medication name, dosage, route of administration, and time of administration.
- Document any patient reactions or side effects.
- Sign and date the documentation.
Effective Communication with Healthcare Team Members
Nurses collaborate with various members of the healthcare team, including doctors, pharmacists, and other healthcare professionals. Effective communication is crucial for sharing important medication-related information, clarifying orders, and discussing any concerns or changes in the patient’s condition. This promotes coordinated care and helps prevent medication errors.
Here are some tips for effective communication with healthcare team members:
- Be clear and concise when communicating medication-related information.
- Use the same terminology as the other healthcare team members.
- Ask questions if you are unsure about anything.
- Document all communication in the patient’s medical record.
Sharing Medication Information with Patients and Their Families
Nurses play a vital role in educating patients and their families about medications. This includes providing information about the purpose of the medication, proper administration techniques, potential side effects, and the importance of adherence to the prescribed regimen. Clear and concise communication helps empower patients to actively participate in their own care and make informed decisions about their medications.
Here are some tips for sharing medication information with patients and their families:
- Use language that the patient and family can understand.
- Be patient and answer any questions the patient or family may have.
- Provide written information about the medication, such as a medication leaflet or a patient information sheet.
In the UK, it is estimated that there are over 237 million medication errors annually, resulting in avoidable harm to patients.
Ensuring Compliance with NMC Standards
Ensuring compliance with the NMC standards for medicines management is crucial in promoting safe and effective care. Nurses, healthcare organizations, and educational institutions must work together to establish a culture of compliance and continuously improve medication management practices.
Here are some ways to ensure compliance with the NMC standards for medicines management:
- Provide education and training on medicines management to all healthcare workers.
- Develop clear and concise policies and procedures for medicines management.
- Regularly review and update medicines management policies and procedures.
- Foster a culture of safety and open communication around medicines management.
- Encourage reporting and learning from medication errors.
By working together, nurses, healthcare organizations, and educational institutions can create a culture of safety and excellence in medicines management. This will ultimately improve patient outcomes and ensure that patients receive the safe and effective care they deserve.
Benefits of Adhering to NMC Standards for Medicines Management
Adhering to NMC standards for medicines management brings numerous benefits to both patients and healthcare professionals. Let’s explore some of these advantages:
Enhanced Patient Safety
Adhering to NMC standards for medicines management significantly enhances patient safety. By following standardized processes for medication administration, documentation, and monitoring, nurses minimize the risk of medication errors and adverse reactions.
Strict adherence to NMC standards ensures that patients receive the right medication, in the correct dosage, through the appropriate route, and at the prescribed time. This reduces the likelihood of medication-related harm and promotes overall patient well-being.
Improved Medication Administration Accuracy
NMC standards emphasize the importance of accurate medication administration. By following guidelines such as the Rights of Medication Administration (right patient, right medication, right dose, right route, right time, right documentation, right response, right to refuse ), nurses minimize the potential for errors during the administration process.
Proper medication administration techniques, including verifying medication orders, using proper dosage calculation methods, and employing safe injection practices, ensure that patients receive their medications safely and effectively.
Optimal Therapeutic Outcomes
Adhering to NMC standards for medicines management contributes to optimal therapeutic outcomes for patients. By closely monitoring medication effects, assessing therapeutic responses, and managing adverse reactions, nurses can make timely interventions to adjust medication regimens as needed.
Consistent and appropriate medication management helps patients achieve the desired therapeutic outcomes, whether it be relieving symptoms, managing chronic conditions, or promoting recovery after surgery or illness. This ensures that patients receive the full benefits of their prescribed medications, leading to improved overall health and quality of life.
Professional Growth and Development
Adhering to NMC standards for medicines management fosters professional growth and development for nurses. By continuously improving their knowledge and skills through education, training, and continuing professional development opportunities, nurses stay up-to-date with best practices in medication management.
Compliance with NMC standards not only enhances nurses’ competence but also demonstrates their commitment to providing safe and high-quality care. This dedication to professional growth and development opens doors for career advancement opportunities, such as specialization in pharmacology or medication safety, further enriching nurses’ professional journeys.
JOIN OUR NEXT MEDICATION TRAINING – SEE NEXT START DATES AND PRICES
Medication Administration Record (MAR) Chart: A Vital Tool for Safe and Effective Care
Medication management is a critical part of providing safe and effective care to patients. As caregivers, it is essential to adhere to the standards set by the Nursing and Midwifery Council (NMC) to ensure the well-being of our patients. One crucial tool that aligns with these standards is the Medication Administration Record (MAR) chart.
What is an MAR Chart?
The MAR chart, or Medication Administration Record, is a document that helps us track and administer medications to patients as prescribed. It supports NMC standards for medicines management by providing a centralized record of medication administration, reducing the risk of errors, and promoting patient safety. You can check the NHS MAR Procedure here: click
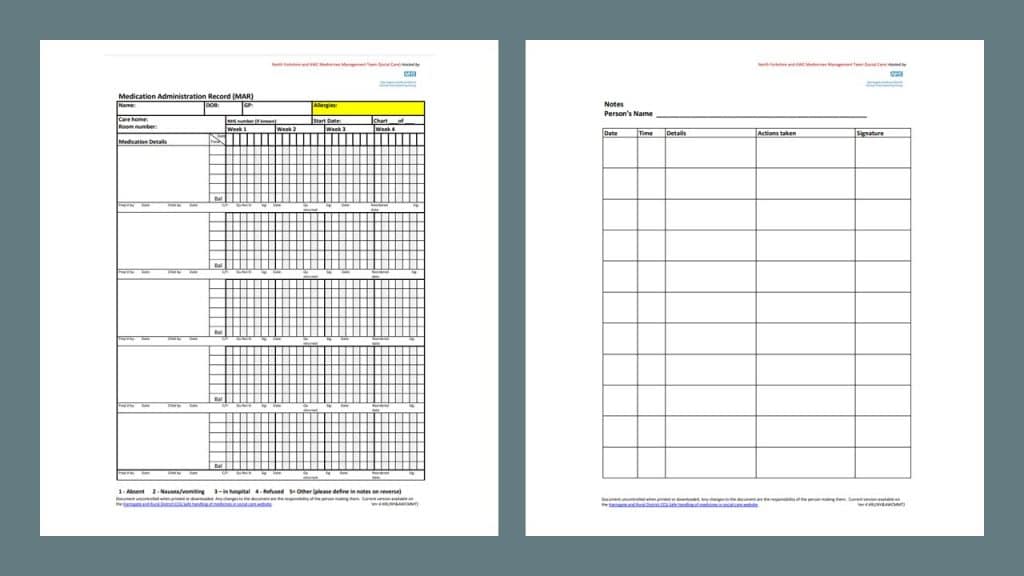

Source: Integrated Care Board
Components of an MAR Chart
The MAR chart has three key components:
Patient Information: The MAR chart includes important details about the patient, such as their name, identification number, and assigned healthcare unit. This helps ensure medications are given to the correct individual.
Medication Details: Within the chart, we find information about prescribed medications, including their names, strengths, dosage instructions, and administration schedule. It gives us a clear overview of the medications prescribed for each patient.
Administration Record: The MAR chart provides a section to document medication administration. It includes spaces to record the date, time, medication name, dosage administered, and the caregiver’s signature or initials. This record helps us keep track of medication administration and maintain accurate documentation.
Aligning the MAR Chart with NMC Standards for Medicines Management
The MAR chart supports NMC standards in several ways:
Enhanced Patient Safety: By utilizing the MAR chart, we can reduce the risk of medication errors and ensure that medications are administered accurately. This aligns with the NMC standard of promoting patient safety and preventing harm.
Effective Communication and Continuity of Care: The MAR chart acts as a communication tool, allowing healthcare professionals to share consistent and accurate information. It facilitates smooth transitions of care between shifts and units, supporting the NMC standard of effective communication and continuity in medication management.
Monitoring Medication Adherence: With the MAR chart, we can closely monitor patients’ medication adherence, identifying any missed doses or irregularities. This helps us intervene promptly and adjust medication regimens when necessary, in line with the NMC standard of ensuring optimal therapeutic outcomes.
Best Practices for Using the MAR Chart
To maximize the benefits of the MAR chart, consider the following practices:
Accuracy and Completeness: Ensure that the MAR chart is accurately and completely filled out. Furthermore verifying patient information, confirming medication details, and promptly documenting medication administration.
Timely Updates: Update the MAR chart in real-time to reflect any changes to the medication regimen. This also includes adjustments in dosages, additions, or discontinuations, as prescribed by healthcare providers.
Regular Review and Reconciliation: Periodically review and reconcile the MAR chart to identify discrepancies or potential errors. This ensures that medication orders match the documented administration.
Things to keep in mind when using MAR Chart
Here are some additional things to keep in mind when using the MAR chart:
- Use the most recent version of the chart. The NMC updates the MAR chart regularly, so it is important to use the most recent version to ensure that you are following the latest standards.
- Be familiar with the chart’s format and instructions. The MAR chart is a complex document, so it is important to be familiar with its format and instructions before you start using it.
- Complete the chart accurately and completely. The MAR chart is a legal document, so it is important to complete it accurately and completely.
- Update the chart as needed. The MAR chart is a dynamic document. It is important to update it as needed to reflect changes in the patient’s medication regimen.
- Review the chart regularly. The MAR chart should be reviewed regularly to identify any potential errors or discrepancies.
See a sample of MAR Checklist below by West Essex Clinical Commissioning Group:
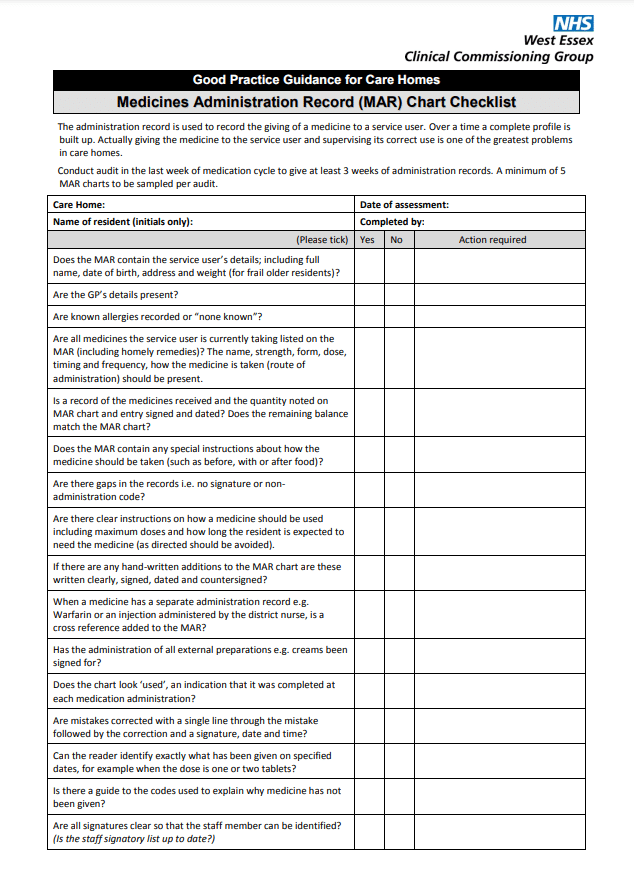
These are some of the steps you can take to ensure that the MAR chart is used effectively to support safe and accurate medication management
As caregivers, adhering to NMC standards for medicines management is crucial for providing safe and effective care. The MAR chart aligns with these standards, supporting accurate medication administration, promoting patient safety, and facilitating communication among healthcare professionals.
By understanding the components of the MAR chart and implementing best practices. We can ensure optimal medication management while upholding the NMC standards, ultimately enhancing patient outcomes and the overall quality of care we deliver.
BECOME AN MEDICATION TRAINER – JOIN OUR NEXT TRAINER COURSES – 01782 563333
Medicine Management Challenges and Future Directions
While adherence to NMC standards for medicines management brings significant benefits, there are challenges that need to be addressed to ensure continued compliance and improvement. Let’s explore some of these challenges and potential future directions:
Addressing Barriers to Compliance
Nurses may face various barriers that hinder full compliance with NMC standards for medicines management. These barriers can include heavy workloads, time constraints, insufficient resources, and inadequate training opportunities.
Healthcare organizations should prioritize addressing these challenges by providing adequate staffing levels, implementing efficient workflow processes, and offering ongoing support and education for nurses.
Embracing Technological Advancements
The future of medicines management lies in embracing technological advancements. Electronic medication administration records, barcode scanning systems, and smart infusion pumps are just a few examples of technologies that can enhance medication safety and streamline documentation processes.
Healthcare organizations should invest in and leverage technology to support nurses in adhering to NMC standards. This includes providing user-friendly technology, offering comprehensive training on its use, and ensuring seamless integration with existing systems.
Promoting Interprofessional Collaboration
Effective medicines management requires collaboration among healthcare professionals. Nurses should actively engage in interprofessional collaboration, working closely with pharmacists, physicians, and other healthcare team members to ensure safe and optimal medication practices.
By fostering a culture of collaboration, open communication, and shared decision-making, healthcare organiSations can overcome silos and promote effective teamwork. This collaboration also extends to engaging patients and their families as active partners in medication management, enhancing patient-centered care and shared accountability.
| Error Stage | Statistics on medication errors in the UK |
|---|---|
| Prescribing | Around 21% of medication errors occur at the prescribing stage |
| Administration | Over 54% of medication errors occur at the administration stage. |
| Dispensing | Around 16% of medication errors occur at the dispensing stage. |
Conclusion on NMC standards for Medicines Management
In conclusion, adhering to NMC standards for medicines management brings numerous benefits, including enhanced patient safety, improved medication administration accuracy, optimal therapeutic outcomes, and professional growth for nurses. Overcoming challenges, such as addressing barriers to compliance, embracing technological advancements, and promoting interprofessional collaboration, is essential for continuous improvement in medication management practices. By prioritizing adherence to these standards, nurses and healthcare organizations contribute to safer, more effective, and patient-centered care.
The NMC standards for medicines management are a valuable resource for nurses and healthcare organizations. By following these standards, we can work together to ensure that patients receive the safe and effective medication management they deserve.
About Caring for Care Training
We are one of the top healthcare training companies within the UK.
We train over 20,000 nurses annually in various courses such as administration of medication training and medical training level 3 within the UK.
As an individual, you can take the option of our face-to-face or blended medication courses within our UK training locations. We do have face-to-face medication trainings in Stoke-on-Trent, London, Epsom, York, Swindon and Warrington.
For organisation who are interested in bespoke medication administration training or any other care training, please contact us. You can call 01782 563333 or send us an email : enquiries@caringforcare.co.uk
People Also Read:
A guide to NMC Revalidation: everything you need to know
Gaining healthcare and nursing competencies
R’s of Medication: How to ensure your staff are administering medication safely
Let us Help you
We’ll help you find the right course for your needs. Tell us a little bit about your situation and what you would like to achieve.
We’ll get back to you within one working day.
